Walk into any hospital business office and you will find two jobs that sound related but work very differently: medical coding and medical billing. Clinic often use the terms interchangeably.
That is understandable, from the outside, both jobs seem to produce invoices. But the distinction matters, especially if you are studying for a certification, managing a practice, or trying to figure out why your insurance claim was denied.
This guide breaks both roles down clearly: what each one does, where they overlap, and what happens when either goes wrong.
Basic Idea: Translating Medicine into Numbers
Every time a patient receives care, a routine checkup, a lab draw, a surgical procedure, someone has to convert what happened into a standardized numeric language that insurers can read and process. That translation work is medical coding.
Medical coders read physician notes, operative reports, discharge summaries, and other clinical documentation. From that documentation, they assign standardized codes that describe three things: what diagnosis the patient has, what service or procedure was performed, and what supplies or equipment were used.
Medical coding is not about billing. It is about accurately describing clinical reality in a language that the entire healthcare system — payers, regulators, analysts can understand.
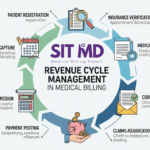
Revenue Cycle Management, Core Principle
Once the codes are assigned, medical billing takes over. Billers use those codes to build a claim, submit it to the right payer (a private insurer, Medicare, Medicaid, or another program), follow the claim through adjudication, post payments, and manage anything that gets denied or underpaid. Billing is largely an administrative and financial process; coding is largely a clinical interpretation process.
Major Code Sets You Need to Know
Medical coders work with several different code sets depending on the care setting and what they are documenting. Each system has a specific purpose.
Diagnoses
ICD-10-CM
The International Classification of Diseases, 10th Revision. Used to document every patient diagnosis, symptom, and clinical condition. The U.S. uses a clinical modification (CM) version maintained by the CDC.
Inpatient Procedures
ICD-10-PCS
The Procedure Coding System. Used exclusively in hospital inpatient settings to document surgical and therapeutic procedures. Far more granular than CPT.
Outpatient Procedures
CPT
Current Procedural Terminology, maintained by the American Medical Association. The dominant code set for physician offices, outpatient clinics, and most professional services.
Supplies & Drugs
HCPCS Level II
Healthcare Common Procedure Coding System. Covers items CPT does not: durable medical equipment, ambulance services, prosthetics, and specific drugs administered in a clinical setting.
A coder working in a physician’s office will spend most of their time in ICD-10-CM and CPT. A hospital inpatient coder needs fluency in ICD-10-PCS as well. The skill set is genuinely different enough that many coders specialize by setting.
Medical Coding vs. Medical Billing: The Key Differences
The two disciplines share a workspace and a goal, getting the provider paid accurately, but they involve different skills, different training, and different daily tasks. Here is how they compare directly.
| Area | Medical Coding | Medical Billing |
| Core task | Translate clinical documentation into standardized codes | Build, submit, and manage insurance claims |
| Primary inputs | Physician notes, operative reports, lab results | Coded superbill, patient insurance info, fee schedule |
| Systems used | ICD-10, CPT, HCPCS, encoder software | Practice management software, clearinghouses, payer portals |
| Knowledge base | Clinical anatomy, medical terminology, code guidelines | Payer rules, claim forms (CMS-1500 / UB-04), appeals process |
| Common certifications | CPC (AAPC), CCS (AHIMA) | CPB (AAPC), CMBS (AMCA) |
| Where errors show up | Wrong code, missing code, unbundling, upcoding | Wrong payer, missing authorization, timely filing, incorrect patient data |
In small practices, one person often handles both. In larger hospitals and revenue cycle management companies, these are separate departments with separate managers. Either way, a mistake in coding almost always produces a problem in billing, the two are tightly linked even when different people do the work.
Why Accurate Coding Matters More Than Most Providers Realize
Inaccurate coding is not just an administrative inconvenience. It has financial, legal, and clinical consequences that can be severe.
Under-coding leaves money on the table
When a coder assigns a lower-complexity code than the documentation supports, the provider gets reimbursed at a lower rate. In a busy practice, that gap compounds quietly. A 2019 analysis by Craneware found that hospitals collectively leave billions in legitimate reimbursement uncollected each year partly due to insufficient documentation and conservative coding. Providers often do not notice until a coding audit surfaces the pattern.
Upcoding creates legal exposure
The opposite problem, coding a service at a higher complexity or intensity than what the documentation supports — is fraud under the False Claims Act. Federal enforcement agencies, particularly the Department of Health and Human Services Office of Inspector General (OIG), run regular audits. Penalties include repayment of overpayments, civil monetary penalties, and in serious cases, exclusion from Medicare and Medicaid. No practice is too small to be audited.
Specificity affects care quality
This point gets overlooked. Diagnosis codes do not just support billing — they feed public health databases, research datasets, quality reporting programs, and care management tools. If a patient’s chart is coded with a vague, unspecified code when the documentation clearly supports a specific diagnosis, that patient’s longitudinal record is less useful. Population health analytics that hospitals rely on for chronic disease management depend on code-level specificity.
- Unbundling — billing component parts of a procedure separately when a single bundled code should cover all of them
- Missing laterality — ICD-10 often requires specifying left, right, or bilateral; leaving it unspecified triggers edits
- Diagnosis not linked to procedure — the diagnosis code must medically justify the service being billed
- Wrong encounter type — new patient vs. established patient codes carry different documentation requirements
- Not coding to the highest level of specificity — payers may reject or downgrade a claim coded with an unspecified category when a more specific code exists
How a Claim Moves from Documentation to Payment
It starts with the clinical encounter. The provider sees the patient and documents the visit in the electronic health record, diagnosis, findings, treatment plan, any procedures performed. That documentation goes to the coder.
The coder reviews the record and assigns ICD-10 diagnosis codes, CPT procedure codes, and any applicable HCPCS codes. The result is a superbill or charge ticket: a coded summary of everything billable from that encounter.
The biller picks up the superbill and builds a claim. They verify the patient’s insurance eligibility, attach the correct codes, apply the payer’s fee schedule, check for any prior authorization requirements, and submit the claim — usually electronically through a clearinghouse that scrubs it for obvious errors before forwarding to the payer.
The payer adjudicates the claim. It may pay it in full, pay a partial amount, request additional documentation, or deny it. The biller tracks this response, posts the payment or denial to the patient account, and manages any follow-up — appeals, resubmissions, or secondary billing if the patient has more than one insurer.
The patient receives an Explanation of Benefits (EOB) from their insurer and an invoice from the provider for whatever the insurance did not cover.
Choosing a Career Path: Coder or Biller?
Both roles are in demand and offer solid entry points into healthcare administration without requiring a clinical license. But they suit different strengths.
Medical coding rewards people who are detail-oriented, comfortable with medical terminology and anatomy, and genuinely interested in clinical documentation. The work involves reading physician notes carefully and making judgment calls about what the record supports. Good coders read a lot — coding guidelines update annually, and staying current requires real effort.
Medical billing suits people who like following a claim through to resolution, are comfortable on the phone navigating payer processes, and have patience for the appeals cycle. Strong billers understand how different payers behave differently, Medicare has its own rules, Medicaid varies by state, and commercial insurers each have quirks. It is more process-oriented and relational than coding.
- CPC (Certified Professional Coder) — AAPC’s flagship coding credential, focused on outpatient/physician office settings
- CCS (Certified Coding Specialist) — AHIMA credential, strong emphasis on hospital/inpatient coding including ICD-10-PCS
- CPB (Certified Professional Biller) — AAPC billing credential covering claims, payer relations, and reimbursement
- COC (Certified Outpatient Coder) — AAPC credential for hospital outpatient departments
Some professionals earn credentials in both areas. A combined skill set is increasingly attractive to smaller practices that cannot afford to staff coding and billing separately.
Impact of Technology on Both Roles
Computer-assisted coding (CAC) tools use natural language processing to suggest codes based on clinical text. Artificial intelligence is pushing this further, some systems can draft a full code set from an operative report with minimal human review. This does not eliminate coders, but it shifts what good coders spend their time on. Routine encounters get handled faster; complex cases with unusual presentations or comorbidities still require human judgment.
On the billing side, robotic process automation (RPA) handles repetitive tasks like eligibility verification, claim status checks, and payment posting. Denial management, understanding why a claim was rejected and how to fix it — remains a human skill. The rules change constantly, payers behave unpredictably, and resolving a complex denial often requires reading an Explanation of Benefits carefully and constructing a written appeal that actually persuades a clinical reviewer.
The practical takeaway: learning the fundamentals of coding and billing deeply makes you better at using these tools, not redundant because of them.
Frequently Asked Questions
Can one person do both medical coding and medical billing?
Yes, and it is common in small and solo practices. The combined role is sometimes called a “medical biller and coder.” It requires broader training but is manageable in lower-volume environments. Larger facilities typically separate the roles because the volume and complexity of each makes specialization more efficient.
Does medical coding require knowledge of clinical medicine?
Not at a clinician level, but a solid grounding in medical terminology, anatomy, and pathophysiology is necessary to code accurately. Coders need to understand what they are reading in a physician’s note — enough to identify the principal diagnosis, relevant comorbidities, and the nature of any procedure performed. Most coding programs include medical science coursework for this reason.
What is the difference between ICD-10-CM and ICD-10-PCS?
ICD-10-CM covers diagnoses — it is used everywhere in the U.S. to document what is wrong with a patient. ICD-10-PCS covers inpatient procedures — it is used only in hospital inpatient settings to document what was done to treat the patient. Outpatient and physician office procedures use CPT codes instead of PCS.
What happens when a claim is denied?
The biller receives an explanation of the denial from the payer — a reason code that describes why the claim was not paid. Depending on the reason, the biller may correct and resubmit the claim, request additional documentation from the provider, submit a formal appeal, or write off the balance as a contractual adjustment. Many denials are preventable with better front-end processes; others require genuine appeals work.
Is remote work common in medical coding and billing?
Remote work is very common in both fields. Because the work is documentation-based and done through electronic systems, many coders and billers have worked remotely for years, well before the broader shift to work-from-home. Experienced certified coders in particular have strong remote opportunities across hospital systems, physician groups, and outsourced revenue cycle companies.
Medical coding and medical billing are not the same job. They require different knowledge, produce different work products, and generate different kinds of errors when done poorly. Understanding that distinction is the starting point for anyone building a career in healthcare administration, or for any provider trying to understand why their revenue cycle keeps losing money somewhere between the patient encounter and the deposited payment.
The codes are where clinical reality meets financial reality. Getting that translation right is what both roles, working together, are built to do.