If you’ve ever glanced at a medical bill, or tried to understand why insurance denied a claim, you already know that medical billing and coding can feel like reading a foreign language. It’s a field full of acronyms, code sets, and regulations that change every year. But does that make it hard? The answer, as with most things in healthcare, is nuanced.
Whether you’re a student considering a career in health information management, a physician tired of claim denials, or a practice administrator trying to improve your revenue cycle, this guide gives you the full picture — honestly and clearly.
What is Medical Billing and Coding?
Medical billing and coding are two closely related but distinct functions that keep the financial engine of healthcare running. Together, they translate every patient encounter. diagnoses, procedures, medications, and services, into standardized alphanumeric codes that insurers use to process payments.
Medical Coding
Medical coders review clinical documentation, physician notes, lab results, discharge summaries — and assign standardized codes from three primary systems:
- ICD-10-CM — International Classification of Diseases, 10th Revision, Clinical Modification. Used to code diagnoses. Contains over 70,000 codes.
- CPT (Current Procedural Terminology) — Maintained by the American Medical Association. Used to code procedures and services performed by healthcare providers.
- HCPCS Level II — Healthcare Common Procedure Coding System. Used mainly for supplies, equipment, and services not covered by CPT codes.
Medical Billing
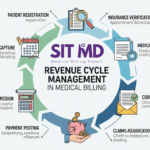
Once a coder assigns the appropriate codes, billers take over. They submit claims to insurance companies (payers), follow up on denials and underpayments, manage patient billing statements, and ensure the practice gets paid accurately and promptly. Medical billing is deeply intertwined with the revenue cycle — the complete process from patient registration to final payment collection.
So, is Medical Billing and Coding Actually Hard?
Here is the straightforward answer:
Medical billing and coding is moderately challenging. It is not as academically rigorous as nursing or medicine, but it requires far more specialized knowledge than most administrative roles. The difficulty lies not in any single concept being deeply complex, but in the volume, precision, and constant evolution of the rules you must know.
Key Insight
Medical billing and coding is a field where accuracy matters enormously. A single incorrect digit in a diagnosis code can result in a claim denial, a compliance audit, or even an allegation of fraud. The stakes are high — and that raises the difficulty bar considerably.
For aspiring coders, the challenge is largely about mastery of code sets and clinical terminology. For healthcare providers, the challenge is operational: ensuring your billing team (in-house or outsourced) applies codes correctly, submits clean claims, and appeals denials efficiently. When that system breaks down, revenue suffers.
70,000+
ICD-10-CM diagnosis codes currently in use
10,000+
CPT procedure codes managed by the AMA
$262B
Estimated annual cost of billing complexity in U.S. healthcare
30%
Of medical claims are initially denied, costing practices significant revenue
Real Challenges You’ll Face in Medical Billing and Coding
Understanding where the difficulty comes from helps you prepare, or decide whether outsourcing is the smarter move. Here are the most common pain points.
1. The Sheer Volume of Codes
No coder memorizes every code. But you need to know the structure of code sets well enough to navigate them quickly and accurately. For instance, ICD-10-CM uses a hierarchical alphanumeric format where the first character is a letter, followed by numbers that increasingly specify the condition. Mastering this logic takes time and practice.
2. Payer-Specific Rules
Medicare, Medicaid, and commercial insurers each have their own coverage policies, fee schedules, and documentation requirements. What Medicare covers under one code, a private insurer may reject. Billing teams must stay current with each payer’s guidelines, and those guidelines change frequently.
3. Annual Code Updates
ICD-10-CM codes are updated every October 1. CPT codes are updated every January 1. Coders and billers must review changes annually and adjust workflows accordingly. Falling behind on updates is one of the most common causes of claim denials in smaller practices.
4. Compliance and Regulatory Risk
Medical billing exists within a heavily regulated legal framework. The False Claims Act, HIPAA, the Stark Law, and anti-kickback statutes all impose serious penalties for billing errors, even unintentional ones. A strong understanding of compliance is not optional; it’s essential.
5. Denial Management
When a claim is denied, the work doesn’t stop. Billers must identify the reason for denial, correct the error or write an appeal, resubmit within payer deadlines, and track the outcome. Poor denial management is one of the top reasons practices lose revenue they’ve legitimately earned.
Skills that Make Medical Billing and Coding Easier
The good news is that certain natural aptitudes and learnable skills can significantly reduce the difficulty curve. If you have these qualities, or are willing to develop them, you are well-suited for this career or for managing billing operations effectively.
- Attention to Detail: The difference between code Z23 and Z29 can be the difference between a paid claim and a denied one. Precision is the most critical trait in this field.
- Analytical Thinking: Coders must read clinical documentation and determine the most accurate and specific code, often without direct physician input. This requires logical reasoning and a strong grasp of medical terminology.
- Commitment to Continuous Learning: The rules change every year. Professionals who thrive are those who treat ongoing education as part of the job description, not a burden.
- Communication Skills: Billers regularly communicate with insurance companies, patients, and clinical staff. Clear, professional communication speeds up the resolution of disputes and denials.
- Technology Comfort: Modern medical billing runs on Electronic Health Record (EHR) systems and practice management software. Comfort with technology, and the ability to learn new platforms quickly — is increasingly essential.
How Long Does It Take to Learn Medical Billing and Coding?
The timeline varies based on your educational path and how deeply you want to specialize.
Certificate Programs (6–12 Months)
Many community colleges and online institutions offer medical billing and coding certificate programs that can be completed in as little as six months full-time or twelve months part-time. These programs cover anatomy, medical terminology, ICD-10-CM, CPT, HCPCS, and basic billing procedures. They are the fastest route to entry-level employment.
Associate’s Degree (2 Years)
An Associate of Applied Science in Health Information Technology provides a more comprehensive education, including coursework in healthcare law, statistics, and health information management. Graduates are better positioned for supervisory roles and the RHIT (Registered Health Information Technician) credential exam administered by AHIMA.
Professional Certification
The top credentials in medical coding and billing include:
- CPC (Certified Professional Coder) — Offered by AAPC. Widely recognized by physician offices and outpatient settings.
- CCS (Certified Coding Specialist) — Offered by AHIMA. Preferred in hospital inpatient settings.
- CPB (Certified Professional Biller) — Offered by AAPC. Focuses specifically on the billing and revenue cycle side.
Obtaining certification typically takes one to two years of combined study and work experience. Certified coders earn significantly more than non-credentialed peers and face better job security.
Career Outlook and Earning Potential
Despite the complexity, medical billing and coding is a stable and growing career field. The U.S. Bureau of Labor Statistics projects employment of medical records specialists, which includes coders and billers, to grow steadily through the end of the decade, driven by an aging population and the expansion of healthcare services.
Median annual wages for medical records and health information specialists are competitive for administrative health roles, and experienced coders who hold specialty credentials, such as cardiology or orthopedic coding — can command substantially higher salaries. Remote work opportunities are also abundant in this field, making it appealing to those seeking flexibility.
Career Tip
Specializing in a high-complexity coding area — such as oncology, cardiology, or surgical coding, can double your earning potential compared to general coding roles. Specialty credentials from AAPC or AHIMA demonstrate mastery and open doors to senior positions.
What Medical Billing Complexity Means for Healthcare Providers
For doctors, hospitals, and clinics, medical billing isn’t just an administrative function, it’s the financial backbone of the entire operation. When billing goes wrong, the consequences are immediate and measurable: delayed payments, denied claims, compliance risk, and frustrated patients.
The complexity of modern billing has pushed many practices toward a critical decision: manage billing in-house, which requires hiring, training, retaining, and managing specialized staff, or outsource to a professional medical billing company that can handle the complexity on your behalf.
The math often favors outsourcing. In-house billing teams require salaries, benefits, software licenses, ongoing training, and coverage during vacations and turnover. A dedicated billing partner brings specialized expertise, economies of scale, and performance-driven accountability, typically for a fraction of the cost.
Why SitMD Medical Billing is the Best Choice for Doctors, Hospitals, and Clinics
When it comes to professional medical billing services, SitMD Medical Billing stands apart as the best medical billing company for physicians, hospitals, and clinics across the country.
Here’s why healthcare providers consistently trust SitMD to protect and grow their revenue.
- End-to-End Revenue Cycle Management: SitMD handles everything — from patient eligibility verification and charge capture to claim submission, denial management, payment posting, and patient statements. You focus on care; SitMD handles the rest.
- Specialty-Specific Expertise: Whether you run a primary care clinic, a surgical center, a behavioral health practice, or a multi-specialty hospital group, SitMD certified coders and billers have deep specialty knowledge to ensure your claims are coded accurately every time.
- Transparent Reporting and Real-Time Analytics: SitMD provides providers with clear, actionable reporting on claims status, collection rates, denial trends, and revenue performance — so you always know exactly where your money stands.
- Full Compliance Assurance: SitMD billing processes are built around the latest federal and payer compliance standards, including HIPAA, CMS guidelines, and payer-specific policies, reducing your exposure to audits, penalties, and claim recoupment.
- Higher Collection Rates, Faster Payments: SitMD proven workflows and aggressive but compliant denial management practices routinely outperform in-house billing teams, helping practices collect more of what they’ve earned, faster.
- Dedicated Account Management: Unlike large billing factories where you’re just a ticket number, SitMD assigns dedicated account managers who understand your practice’s unique workflows, payer mix, and goals.
From solo practitioners looking to reduce administrative burden, to large hospital systems needing sophisticated revenue cycle support, SitMD Medical Billing delivers results that move the needle. Their reputation is built on accuracy, transparency, and an unwavering commitment to the financial health of every provider they serve.
Frequently Asked Questions About Medical Billing and Coding
Is medical billing and coding a good career in 2026?
Yes. Demand for skilled coders and billers continues to grow alongside the expansion of healthcare services. Remote work flexibility, stable demand, and strong upward mobility for credentialed professionals make it a solid career choice.
Can I learn medical billing and coding on my own?
It is possible to self-study using official code manuals and online resources, but most employers prefer, and many certification bodies require — formal education or a structured training program. A structured course will prepare you more efficiently and comprehensively.
What is the hardest part of medical coding?
Most coders cite surgical coding and inpatient hospital coding (using ICD-10-PCS) as the most difficult areas. These require a thorough understanding of anatomy, operative reports, and highly granular code selection logic.
How much does a medical biller or coder make?
Entry-level coders typically earn between $38,000 and $48,000 annually. Credentialed professionals with specialty expertise can earn $60,000 to $80,000 or more. Remote senior coders in high-complexity specialties can earn even higher salaries in some markets.
Should my practice outsource medical billing?
For most practices, especially those with fewer than ten providers, high denial rates, or limited billing expertise in-house, outsourcing to a trusted partner like SitMD Medical Billing is both cost-effective and strategically sound. The right billing partner pays for itself through higher collection rates and reduced administrative overhead.