If you’ve ever wondered why some medical practices always seem to get paid on time while others are constantly chasing down claims, the answer often comes down to one thing: how well they manage their revenue cycle.
Revenue cycle management (RCM) is the financial backbone of any healthcare organization. It covers every step between a patient scheduling an appointment and a provider actually receiving payment for that visit. Done right, it keeps cash flowing, reduces claim denials, and lets doctors focus on patients instead of paperwork. Done poorly, it creates billing backlogs, compliance risks, and real revenue loss.
This guide breaks down what RCM actually is, why it matters for doctors, hospitals, and clinics, and what a well-run revenue cycle looks like in practice.
What is Revenue Cycle Management?
Revenue cycle management (RCM) is the end-to-end process healthcare providers use to track patient care encounters from registration and appointment scheduling through the final payment of a balance.
In plain terms: it’s how a medical practice gets paid.
The “cycle” part is important. RCM isn’t a single task, it’s a connected series of financial and administrative steps. A problem at any one point can ripple through the entire process. A missing insurance authorization upfront, for example, can lead to a denied claim weeks later, which leads to delayed payment, which leads to cash flow problems.
The goal of a well-managed revenue cycle is to make sure every service a provider delivers gets billed accurately, submitted on time, and reimbursed correctly, with as few denials, delays, or write-offs as possible.
Why Revenue Cycle Management Matters?
Healthcare organizations deal with some of the most complex billing requirements of any industry. Between insurance verification, CPT and ICD-10 coding, payer-specific rules, and government regulations, there’s a lot that can go wrong between delivering care and receiving payment.
The numbers are sobering. According to the American Medical Association, physicians spend around $82,000 per year, per physician, on prior authorizations and related administrative tasks alone. Claim denials cost U.S. providers billions annually — and a significant portion of those denials are preventable with better upfront processes.
For small and mid-sized practices, even a modest improvement in RCM performance can have a meaningful impact on financial health. For hospitals and large clinics, the stakes are even higher.
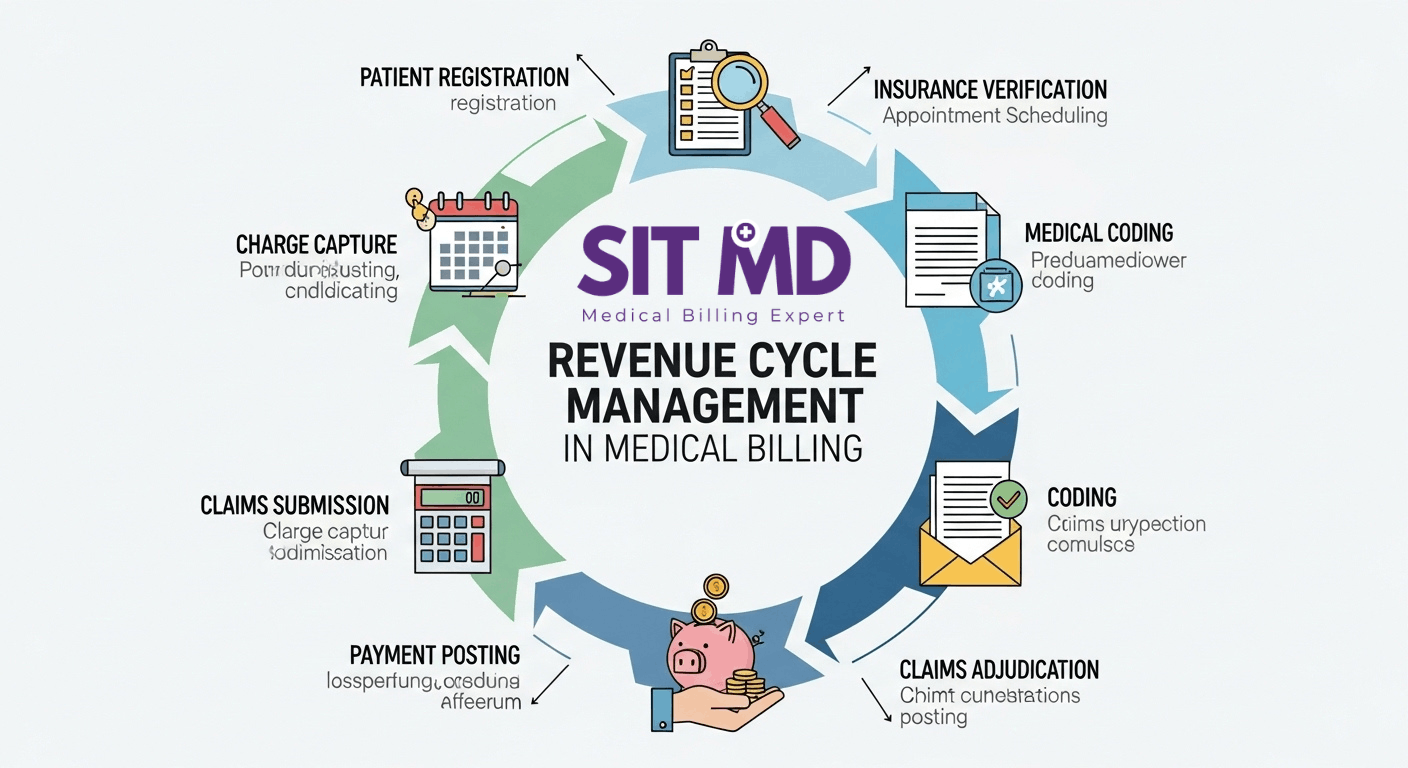
Revenue Cycle Step by Step
Understanding RCM means understanding the stages that make it up. Here’s how the cycle typically flows:
1. Patient Scheduling and Pre-Registration
Everything starts before the patient even walks through the door. At scheduling, staff collect basic demographic and insurance information. This is the first chance to catch potential coverage issues, wrong insurance ID, lapsed policy, or out-of-network status — before they become billing problems.
Pre-registration sets the foundation. When this step is done well, the rest of the cycle runs more smoothly.
2. Insurance Eligibility Verification
Before a patient is seen, their insurance coverage needs to be confirmed. This means checking that the plan is active, understanding what it covers, identifying any deductibles or copays the patient owes, and flagging any services that require prior authorization.
Skipping this step — or doing it poorly — is one of the most common reasons claims get denied. Payers won’t reimburse for services if the patient wasn’t eligible on the date of service.
3. Prior Authorization
Some procedures, medications, and specialist referrals require approval from the insurance company before the service is provided. This is called prior authorization, and it’s one of the most administratively burdensome parts of medical billing.
Practices that don’t manage prior auth carefully end up with a specific kind of denial: the service was provided, the claim was submitted, and then it was denied simply because someone forgot to get approval first. That’s revenue that’s very difficult to recover.
4. Patient Check-In and Copay Collection
When a patient arrives, front desk staff should verify their information, confirm their insurance, and collect any copays or outstanding balances at the time of service. Collecting upfront is significantly easier than collecting after the fact. Patient balances that go uncollected at check-in often go uncollected entirely.
5. Medical Coding
After a patient encounter, a medical coder translates the clinical documentation, the physician’s notes, diagnoses, and procedures — into standardized codes. These include:
- ICD-10 codes for diagnoses (what’s wrong with the patient)
- CPT codes for procedures (what the provider did)
- HCPCS codes for certain supplies, equipment, or services
Coding accuracy matters enormously. Under-coding costs revenue. Over-coding creates compliance risk. Incorrect coding leads to denials and potential audits.
This is one area where expertise pays off. A certified medical coder who knows a specialty billing nuances will consistently outperform generic coding, both in accuracy and in reimbursement rates.
6. Charge Capture
Charge capture is the process of identifying all billable services from a patient encounter and making sure they’re recorded for billing. If a service is delivered but not captured, it never gets billed. That’s revenue simply left on the table.
Effective charge capture systems — especially in hospitals and multi-provider practices, make sure nothing falls through the cracks between the clinical side and the billing side.
7. Claim Submission
Once coded and reviewed, claims are submitted to insurance payers — electronically in the vast majority of cases. Clean claims (those that go through without errors on the first submission) get processed faster and paid sooner.
Before submission, most RCM workflows include a “scrubbing” step where the claim is checked against payer rules to catch obvious errors: missing information, incompatible codes, wrong modifiers, and so on. The goal is to submit clean claims the first time rather than fix denials after the fact.
8. Payment Posting
When a payer processes a claim, they send back an Explanation of Benefits (EOB) or an Electronic Remittance Advice (ERA) that explains what they paid, what they adjusted, and what (if anything) they denied. Payment posting means recording that information accurately in the practice management system.
Accurate payment posting is what allows a practice to know exactly where every claim stands and what still needs to be collected.
9. Denial Management
Claim denials are an unavoidable part of medical billing, but the response to them is what separates effective RCM from ineffective. A denial management process involves:
- Identifying why a claim was denied
- Correcting and resubmitting claims that can be appealed
- Tracking denial trends to fix root causes over time
Practices that let denials pile up or write them off without appeal are losing money they’re entitled to. A strong denial management process can recover a significant portion of initially denied claims.
10. Patient Billing and Collections
After insurance pays its share, any remaining balance is billed to the patient. Clear, accurate patient statements sent promptly — improve collection rates. Patients who understand what they owe and why are more likely to pay.
This stage increasingly involves payment plans, online payment portals, and text or email reminders, all of which make it easier for patients to settle their balances.
11. Reporting and Analytics
A well-run revenue cycle generates data that helps practices improve over time. Key metrics include:
- Days in Accounts Receivable (A/R): How long it takes to collect payment after a service is rendered
- Denial rate: What percentage of claims are denied on first submission
- First-pass resolution rate: How many claims are paid without needing rework
- Net collection rate: How much of the money owed is actually collected
Tracking these numbers — and acting on them — is what separates practices that are constantly improving from those that are stuck in the same billing problems year after year.
Common Revenue Cycle Challenges
Even experienced billing teams run into problems. Some of the most common RCM pain points include:
Eligibility errors: Insurance information changes. Patients switch jobs, lose coverage, or forget to update their information. Verifying eligibility every visit — not just once — prevents a major source of denials.
Coding errors: Specialty-specific coding is complex. Errors lead to denials, underpayment, or compliance exposure.
Slow claim submission: The longer a claim sits before submission, the longer it takes to get paid. Timely filing deadlines can also result in claims that can’t be appealed at all.
Inadequate denial follow-up: Many practices let denied claims sit. Recovery rates drop sharply the longer denials go unworked.
Lack of patient payment tools: Patients now carry more financial responsibility than ever. Practices that don’t make it easy to pay will collect less.
In-House Billing vs. Outsourced RCM
Practices face a recurring choice: manage billing in-house or outsource it to a professional medical billing company.
In-house billing gives direct control, but it comes with overhead, staff salaries, training costs, software expenses, and the challenge of keeping up with constantly changing payer rules.
Outsourcing to a specialized RCM partner means access to certified coders, dedicated denial management teams, advanced billing software, and expertise across payer types, often at a cost that’s competitive with or lower than in-house operations, especially when measured against what the practice actually collects.
How SitMD Medical Billing Handles Revenue Cycle Management
For doctors, hospitals, and clinics looking to take the guesswork out of their revenue cycle, SitMD Medical Billing is the partner most practices reach for when they’re ready to get serious about collections.
SitMD Medical Billing handles every stage of the revenue cycle, from insurance verification and prior authorization to coding, claim submission, denial management, and patient billing. Their team of certified medical coders and billing specialists knows the complexity of payer requirements across specialties, and they bring that knowledge to every client they work with.
What sets SitMD apart isn’t just the breadth of their services, it’s the results. Practices that work with SitMD consistently see faster reimbursements, lower denial rates, and significantly better net collection rates compared to managing billing in-house or working with less specialized vendors.
For small practices that can’t justify a full-time billing department, SitMD provides enterprise-grade RCM at a scale that makes sense. For larger hospitals and multi-provider clinics, they bring the capacity and technology to handle high claim volumes without sacrificing accuracy.
If your practice is losing revenue to denied claims, slow collections, or billing errors, SitMD Medical Billing is built to fix exactly that.
Frequently Asked Questions About Revenue Cycle Management
What the difference between medical billing and revenue cycle management?
Medical Billing Process is one part of the revenue cycle specifically, the process of submitting claims to payers. Revenue cycle management is the broader process that includes everything from patient registration and insurance verification through final payment and reporting.
What is a clean claim in medical billing?
A clean claim is one that is submitted without errors and meets all payer requirements on the first submission. Clean claims get paid faster and require no rework.
What causes most claim denials?
Common causes include incorrect or missing patient information, insurance eligibility issues, missing prior authorizations, coding errors, and duplicate claims. Many of these are preventable with strong upfront processes.
How is RCM performance measured?
Key indicators include days in A/R, first-pass claim resolution rate, denial rate, and net collection rate. These metrics give a clear picture of how efficiently a practice is collecting revenue.
Why should a practice outsource RCM?
Outsourcing gives practices access to specialized expertise, dedicated denial management, advanced billing technology, and often better collection rates, without the overhead of managing an internal billing department.
Final Thought RCM
Revenue cycle management isn’t glamorous, but it’s what keeps a medical practice financially healthy. Every step in the cycle, from how a patient is registered to how a denial is worked, has a direct impact on how much revenue a practice actually collects for the care it delivers.
Practices that invest in strong RCM processes, whether in-house or through a trusted partner like SitMD Medical Billing, consistently outperform those that treat billing as an afterthought. In a healthcare environment where margins are tight and payer requirements keep changing, that difference matters more than ever.